Innovative injury services
From Diagnosis To Performance
Neil Liffen offers services across the east of england
MAKE YOUR FIRST STEP IN IMPROVING YOUR WELLBEING
Welcome To My Practice
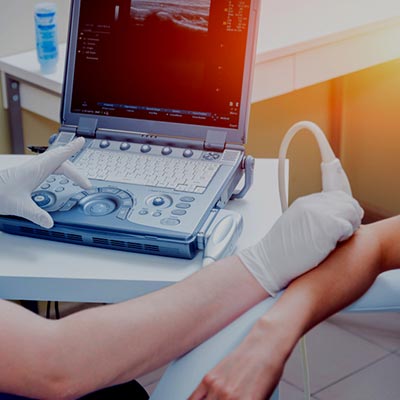
Welcome. Neil Liffen’s unique selling point is his expertise in diagnostic ultrasound scanning and this is available at every appointment.
In correlating the findings from an orthopaedic examination with diagnostic ultrasound scan he arrives at your diagnosis.
A correct diagnosis correct greatly enhances your success in managing your injury efficiently, offering benefits of reassurance, saving time and money.
These services are offered at multiple clinics and at some of the most respected clinics in the east of England.

Neil Liffen
Extended Scope Physiotherapist and MSK Sonographer.
HOW DOES IT ALL WORK
Consultation Process
services available
My Services
DON’T TAKE OUR WORD FOR IT
Client Reviews
“I was having a very frustrating time of shoulder pain and despite several failed treatments from other clinicians I visited Neil Liffen for a diagnostic ultrasound. He was able to perform a diagnostic ultrasound on my first session, and explain to me in detail the problems with my shoulder. He then explained the treatments options and we have now discussed the optimal management pathway for my shoulder. Now I have a specific diagnosis, I have some direction! I am extremely happy with the service provided.“
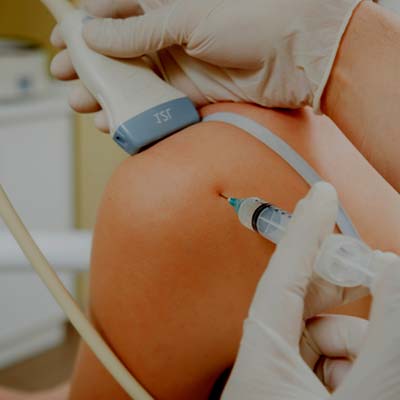
“I would highly recommend Ostenil injections (hyaluronic acid) by Neil Liffen for knee osteoarthritis. I have yearly Ostenil injections which help settle my knee pain and improves function.“
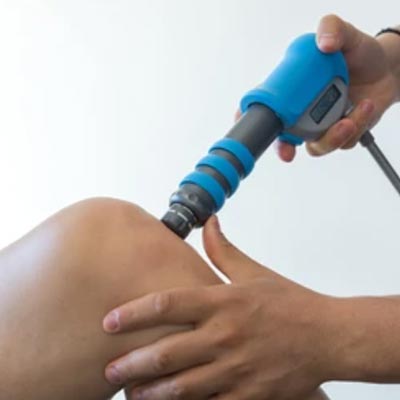
“I suffered with heel pain for over a year. I was so frustrated having seen many clinicians and not having a formal diagnosis and failed treatments. I was recommended to see Neil Liffen from a colleague, who performed a diagnostic ultrasound, which Neil explained very clearly and compared to my good side a s a comparison. I found this extremely helpful to understand the condition. He then recommended shockwave therapy which was very tender during treatment but gave me immediate relief. I had four treatments and I was pain-free. Neil also encouraged me to perform a loading rehabilitation program, which has worked brilliantly. I would recommend his services.“